The Great Reality Check Part 5: Acute fractures of the arms and legs
Read the results of our new user studies – up-to-date and transparent!
Purpose:
The aim of the study was to prospectively assess the performance of a common AI assistant for fractures of the arms and legs, validated with the first read reports of radiologists specialized in emergency radiology as well as imaging and clinical follow-up.
Patients, Materials and Methods:
In late 2025, 140 patients (age: 18 to 81 years, mean: 42 years, standard deviation: ± 20 years) who had been referred to ERS Emergency Radiology Schueller, a provider of teleradiology services, for reporting radiographs of the peripheral skeleton due to suspected acute fracture of the arms or legs, were randomly and prospectively enrolled in the study over 12 consecutive weeks. The radiographs of these patients were evaluated using the AI assistant BoneView (Gleamer, Saint-Mandé, France). Radiologists reported the radiographs without the initial knowledge of the AI results and compared the radiological with the AI findings in a second step. Gold standard were the specialists´ reports as well as imaging and clinical follow-up. In case of discrepancies between the radiologists´ and the AI assistants´ findings, radiographs were second read within 30 minutes at the latest.
Results:
Of 140 patients, 2 AI results, one each of the arms and one of the legs, could not be retrieved. Radiologists and clinical follow-up diagnosed acute 66 fractures (47%) in 138 patients, including 18 arm fractures in 57 patients (31.5%; total 13%) and 48 leg fractures (59.2%; total 34%) in 81 patients. The results yielded by the AI assistant are given for fractures of the arms in Table A, for fractures of the legs in Table B. Table C shows the overall result; true positive (TP), false positive (FP), false negative (FN), and true negative (TN) in absolute numbers; sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) in percent.
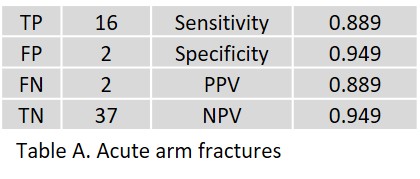 In acute arm fractures, 2 FP of the proximal radius and the scaphoid were observed (ages 78 and 65 years, respectively). Two FN with minor radiolucency lines of the distal clavicle as well as the posterior circumference of the humeral head were observed, which were confirmed as fractures in radiological and clinical follow-up.
In acute arm fractures, 2 FP of the proximal radius and the scaphoid were observed (ages 78 and 65 years, respectively). Two FN with minor radiolucency lines of the distal clavicle as well as the posterior circumference of the humeral head were observed, which were confirmed as fractures in radiological and clinical follow-up.
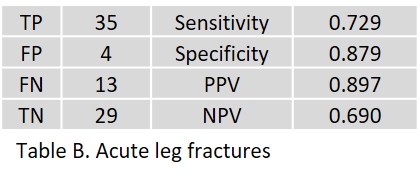 In acute leg fractures, 4 FP of the femoral neck, greater trochanter (age: 71 and 80 years, respectively), lateral tibial plateau (age: 52 years), and navicular bone (age: 76 years) were observed. Thirteen FNs included short, small avulsions of the talus (age 49 to 73 years), nondisplaced Weber A fractures of the distal fibula (age 28 to 46 years), a minimal fracture of the navicular bone (age 25 years), and a small subtrochanteric avulsion of the proximal femur (age 79 years).
In acute leg fractures, 4 FP of the femoral neck, greater trochanter (age: 71 and 80 years, respectively), lateral tibial plateau (age: 52 years), and navicular bone (age: 76 years) were observed. Thirteen FNs included short, small avulsions of the talus (age 49 to 73 years), nondisplaced Weber A fractures of the distal fibula (age 28 to 46 years), a minimal fracture of the navicular bone (age 25 years), and a small subtrochanteric avulsion of the proximal femur (age 79 years).
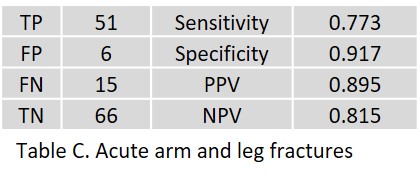 Table C shows the overall result.
Table C shows the overall result.
Discussion:
The AI assistant yielded 15 FN (10.9%) and 6 FP (4.3%) out of 138 FP (27%) with significantly better performance on acute arm fractures (FN and FP 3.5% each) than on acute leg fractures (FN 16%, FP 4.9%). The overall result is therefore revised slightly downwards. The AI assistant proved to be particularly reliable in the differential diagnosis of periarticular calcifications and joint effusions. Displaced fractures were consistently TP on the arms and legs. The specificity is slightly lower than the impressions we published on this platform on May 25, 2023. The high sensitivity is comparable (see https://www.radailogy.com/comprehensive-ai-fracture-diagnosis-of-the-peripheral-skeleton/). In summary, our study shows that the AI assistant is of great use in acute fractures of the peripheral skeleton, especially the arms, in particular for the first review of the radiographs by trauma physicians. The AI assistant can also be used successfully in teleradiology with the continued need for double-checking by experienced emergency radiologists.
Gerd Schueller and the Radailogy Team

